Find Peace Between The Sheets
Hormonal changes can bring on insomnia, or make it worse. But Midi's expert clinicians address the root causes with targeted solutions.


Hormonal changes can bring on insomnia, or make it worse. But Midi's expert clinicians address the root causes with targeted solutions.
Midi is available in all 50 states, with insurance coverage for virtual visits and prescriptions.

Sleep issues affect up to 47 percent of women during perimenopause, and 60 percent after menopause². Hormonal changes, menopausal symptoms like hot flashes, and age-related sleep conditions are among the issues keeping us up at night.
Here’s the good news: Solving sleep issues benefits every part of your health, from your weight to your heart and brain—and our clinicians have the tools to help.
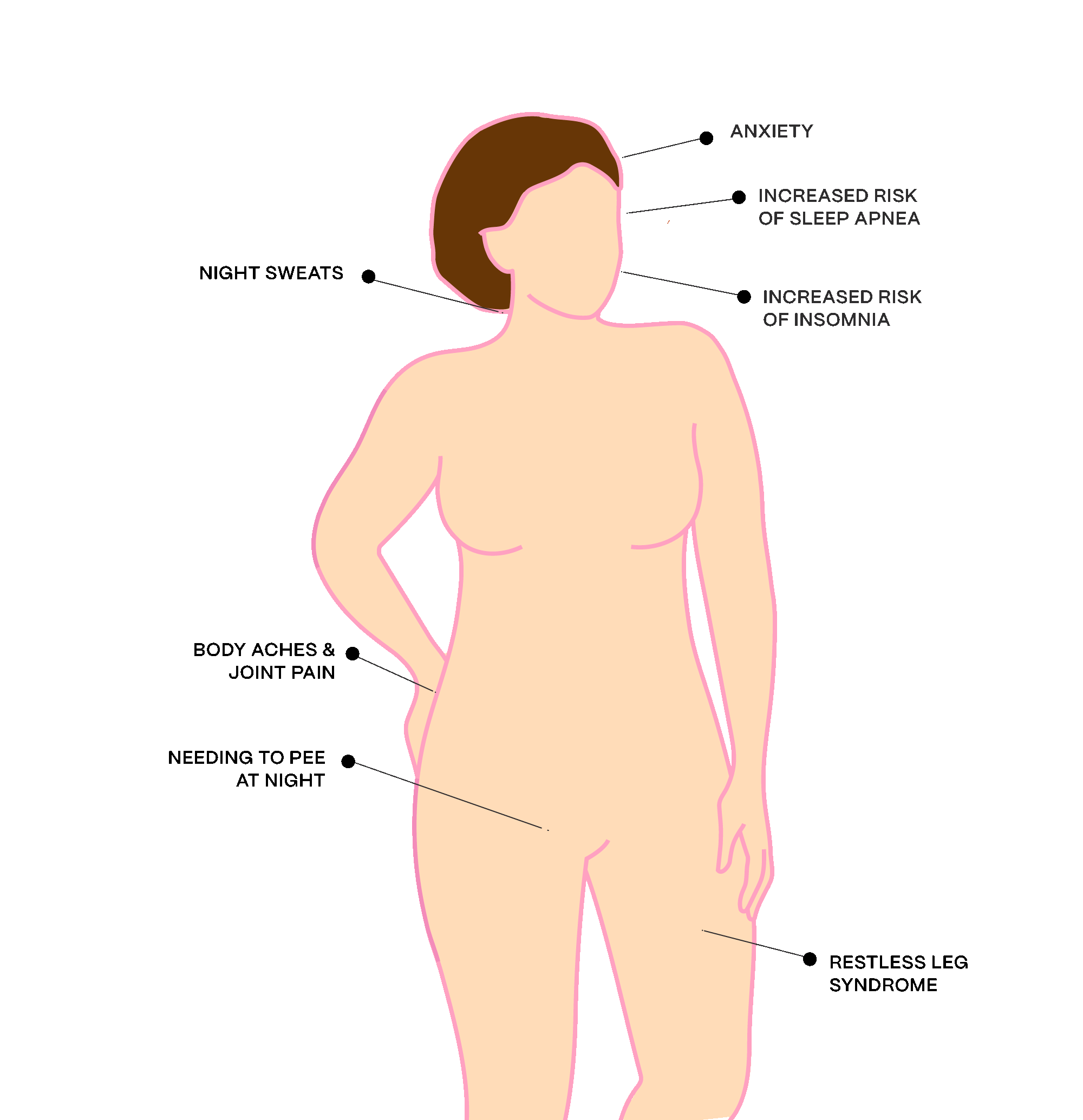
Our expert clinicians offer a suite of solutions to support your shut eye, so you wake up rested every morning and experience life without exhaustion.
Wherever you are in your journey, we’ll meet you there with the solutions you need.

Only pay your standard co-pay and deductible
Only pay standard co-pay and deductible
$250
$150
Midi is in-network with most PPO plans. Coverage varies by plan; deductibles, coinsurance, and copays may still apply. Midi Health and the Medical Groups are not enrolled with and are not participating providers with state healthcare programs (i.e., Medi-Cal, Medicaid). We cannot treat Medicaid or Medi-Cal patients at this time, even as self-pay patients.
Midi is not covered by Medicare or any Medicare-related insurance plan. Midi can accept Medicare beneficiaries as self-pay patients, but beneficiaries cannot submit any claims related to their Midi visits, medications, or associated services. Have questions about insurance or anything else? Email us at support@joinmidi.com and our support team will jump in to help.