Insurance-Covered Hormone Replacement Therapy
Hormone replacement therapy offers the most effective relief for many menopause and perimenopause symptoms, helping women feel better within weeks, even days.
Midi’s hormone specialists prescribe HRT safely, and that starts with an in-depth virtual visit to determine if HRT is right for you.
Join more than 230,000 women who love and trust Midi for their midlife care.

Accepted by Insurance, Nationwide
Virtual visits with a Midi clinician—plus prescriptions in your Care Plan—are covered by major insurance providers across the country. Confirm your coverage by selecting your state below.

Midi is in-network with most PPO plans. Coverage varies by plan; deductibles, coinsurance, and copays may still apply. Midi Health and the Medical Groups are not enrolled with and are not participating providers with state healthcare programs (i.e., Medi-Cal, Medicaid). We cannot treat Medicaid or Medi-Cal patients at this time, even as self-pay patients.
Midi is not covered by Medicare or any Medicare-related insurance plan. Midi can accept Medicare beneficiaries as self-pay patients, but beneficiaries cannot submit any claims related to their Midi visits, medications, or associated services.
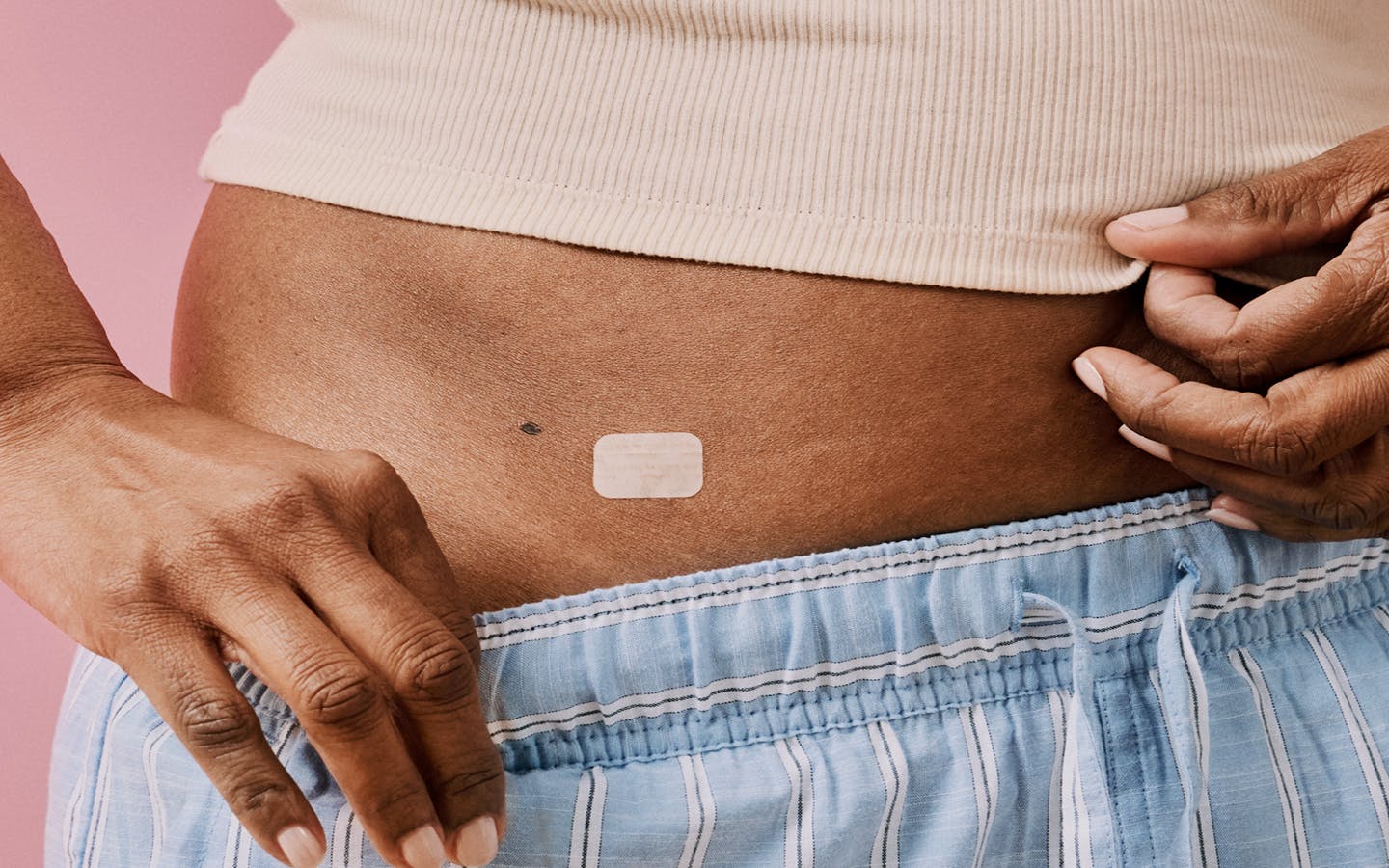
How Hormone Replacement Therapy Works
When hormone levels drop during the menopause transition, you can experience symptoms from head to toe. HRT replenishes just enough estrogen and progesterone to bring you relief.
True Stories Of Transformation
Expert Care.
Sane Pricing.
Initial Visit
Only pay your standard co-pay and deductible
Continued Care Visits
Only pay standard co-pay and deductible
Initial Visit
$250
Continued Care Visits
$150
Midi is in-network with most PPO plans. Coverage varies by plan; deductibles, coinsurance, and copays may still apply. Midi Health and the Medical Groups are not enrolled with and are not participating providers with state healthcare programs (i.e., Medi-Cal, Medicaid). We cannot treat Medicaid or Medi-Cal patients at this time, even as self-pay patients.
Midi is not covered by Medicare or any Medicare-related insurance plan. Midi can accept Medicare beneficiaries as self-pay patients, but beneficiaries cannot submit any claims related to their Midi visits, medications, or associated services. Have questions about insurance or anything else? Email us at support@joinmidi.com and our support team will jump in to help.